Medical Disclaimer: The following content should not be used as medical advice or as a recommendation for any specific treatment. It is important to consult your health care provider prior to starting a new treatment or altering your current treatment plan.
Expiratory positive airway pressure (EPAP) devices may be used to treat obstructive sleep apnea (OSA). OSA is a common sleep-related breathing disorder that affects around 10% to 30% of U.S. adults. And data suggests that the prevalence of OSA continues to rise.
People with OSA experience paused or reduced airflow during sleep due to a blocked or narrowed airway. This disordered breathing can result in sleep interruptions that may cause people to feel tired throughout the day.
When left untreated, OSA may increase the risk of medical problems such as high blood pressure. OSA may also increase the likelihood of accidents when driving.
Because of the sleep interruptions and related risks, treating OSA is important. EPAP therapy is one of several treatment options available. We explore how EPAP therapy works and how it differs from continuous positive airway pressure (CPAP) therapy and other common OSA treatments.
What Is EPAP Therapy?
EPAP therapy involves wearing a lightweight device on the nose during sleep to treat obstructive sleep apnea. An EPAP device contains two valves that are inserted into the nostrils. Some models also require a strap that goes around the head to keep the device in place. EPAP devices leverage the sleeper’s breathing to create resistance during exhales.
EPAP devices allow a sleeper to breathe in as they normally would. Then, the valves create resistance as the sleeper breathes out. This pressure makes the airway less likely to become narrowed or obstructed on the next inhaled breath.
A clinical trial demonstrated that EPAP therapy can reduce the number of times a person with OSA experiences lapses or reductions in breathing during sleep. People using EPAP therapy were also found to experience fewer nighttime awakenings and less snoring. However, additional studies need to be conducted for researchers to know how EPAP compares to CPAP and other available treatments for sleep apnea.
How Is EPAP Different from CPAP Therapy?
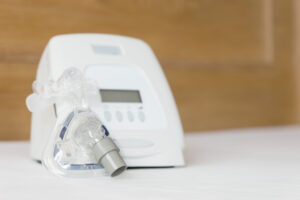
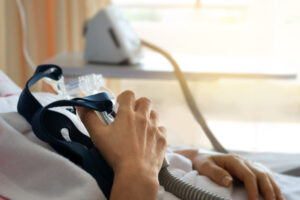
CPAP therapy is the standard treatment prescribed for OSA. CPAP machines work by delivering a steady flow of air to keep the airway open during sleep.
EPAP is considered an alternative treatment for OSA that may be helpful for people who struggle to use their CPAP machines. It differs from CPAP therapy in a few ways.
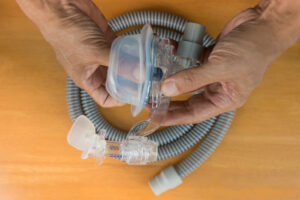
- Use: EPAP therapy involves inserting small valves that provide resistance into the nostrils. In contrast, CPAP treatment involves wearing a mask over the nose or both the nose and mouth. The CPAP machine delivers air into a hose connected to the mask, keeping the airway open.
- Operation: EPAP devices are lightweight and quiet. They do not release air or require an external power source. CPAP machines must be either plugged into an electrical outlet or battery-powered. CPAP machines can emit noise that may make it hard for some people to sleep.
- Maintenance: Some EPAP devices are designed for single use, while others can be reused. Reusable EPAP devices should be cleaned after each use and replaced every three months. Similarly, the CPAP mask and tube should be cleaned regularly and replaced every three to six months.
- Air pressure setting: Adjusting the setting on a CPAP device often requires a health care provider. EPAP devices do not require air pressure adjustments, since they do not emit air.
- Side effects: Both EPAP and CPAP therapies are associated with mild side effects. EPAP therapy may cause nasal discomfort, dry mouth, headache, and trouble sleeping. CPAP therapy is also associated with nasal dryness and irritation.
- Ease-of-use: Doctors often need to educate people with OSA on how to use a CPAP machine. Similarly, education is needed for EPAP therapy, but some people find EPAP devices easier to use.
Who Is EPAP Best for?
People who cannot tolerate CPAP therapy may benefit from an alternative treatment option like EPAP therapy. Although CPAP therapy is the primary treatment given for OSA, not everyone prescribed CPAP therapy uses it as often as recommended. When a person with OSA stops using a CPAP machine, symptoms generally return within a few days.
Experts estimate that up to half of people prescribed a CPAP machine find it challenging to sleep with the device. Reasons people may discontinue using CPAP therapy include discomfort with how their mask fits and side effects such as nasal discomfort and skin irritation.
In contrast, people who are prescribed EPAP therapy report using the device regularly, which makes it a favorable alternative for those who can’t tolerate CPAP.
Studies suggest that people who have mild to moderate OSA without any major underlying health problems may be the ideal candidates for EPAP treatment. However, more research is needed to identify who can benefit most from EPAP.
Deciding Which Therapy Is Right for You
Although CPAP therapy is ideal for people with severe obstructive sleep apnea, those with mild to moderate OSA who cannot tolerate using a CPAP machine may benefit from alternative treatments like EPAP therapy.
If you’ve been diagnosed with OSA and have trouble using a CPAP machine, speak with a doctor to explore other treatment options, like EPAP therapy. Additional OSA treatment options may also include oral appliances, surgery, or lifestyle changes, like losing weight, sleeping in a different position, or reducing alcohol and sedative use.
Certain factors, such as your medical history, sleep habits, OSA severity, and the shape of your airway or tonsils may determine which treatment option is best for your needs.
- Oral appliances: Oral appliances are devices that reposition the jaw or move the tongue forward. Although not as effective as CPAP therapy, they can help relieve snoring and mild OSA. A dentist or health care professional typically custom fits the oral appliance, which should be worn each time you sleep.
- Surgery: Surgical intervention is typically the last resort used when other non-surgical methods fail to improve OSA. There are different types of procedures used to correct airway abnormalities causing OSA.
- Positional therapy: Some studies suggest that sleep position therapy may help with treating OSA. Specifically, side sleeping may be beneficial for people who have sleep apnea symptoms while back sleeping.
Many people who are treated for OSA experience improved sleep quality and duration, along with increased productivity. Regardless of which treatment your doctor recommends, being treated is most important.
Frequently Asked Questions About EPAP Therapy
The U.S. Food and Drug Administration (FDA) has approved certain prescription EPAP devices to treat people with mild to moderate obstructive sleep apnea.
There are also non-prescription EPAP devices available for sale, but they are only intended to treat snoring, not FDA-approved to treat OSA.
Initial studies show that EPAP therapy can reduce nighttime snoring. However, it is important to discuss your symptoms with your health care provider. They can help you determine the best course of treatment for snoring and other sleep disruptions.
EPAP therapy may benefit you if you have OSA and cannot tolerate CPAP therapy. However, many people with OSA are not aware that they have the condition. Speak with a doctor if you suspect you may have a sleep disorder, regularly wake up feeling tired, or receive complaints about your loud snoring.
In preliminary studies, EPAP therapy has been found to reduce how often people with OSA pause or slow breathing while asleep. People who use EPAP devices also report reduced daytime tiredness and improvements to quality of life and sleep. However, more research is needed to understand how EPAP therapy compares to other established sleep apnea treatments.
Common side effects from EPAP therapy are difficulty breathing out while wearing the device, headaches, dry mouth, and discomfort in the nose. Discuss potential risks and side effects with your doctor before starting any OSA treatment.
The latest research suggests people who have mild to moderate OSA and no major underlying health conditions are likely the ideal candidates for EPAP therapy. However, more long-term clinical studies are needed to better understand who would be the ideal candidate for EPAP therapy.
Coverage for OSA treatment will depend on your insurance plan. Some insurers have pre-authorization policies for OSA treatments and diagnostics tests. Medicare may cover a three-month trial period for CPAP therapy for specific patients.
References
Ask the Sleep Doctor
Have questions about sleep? Submit them here! We use your questions to help us decide topics for future articles, videos, and newsletters. We try to answer as many questions as possible. You can also send us an email. Please note, we cannot provide specific medical advice, and always recommend you contact your doctor for any medical matters.