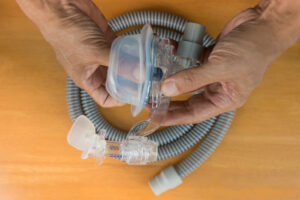
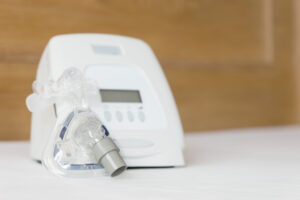
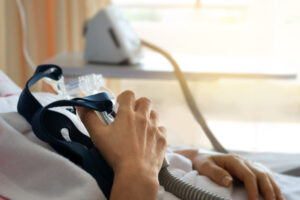
Continuous positive airway pressure (CPAP) machines keep the upper airway open by pumping a constant stream of pressurized air into the airway through a mask. Most people receiving CPAP therapy use pressure levels between 8 and 10 cm H20, but the best level varies from person to person.
CPAP is a highly effective treatment for obstructive sleep apnea (OSA) if used consistently. Before you can begin to benefit from CPAP, your health care team must find out what the right CPAP pressure setting is for your situation.
The optimal setting for CPAP is the lowest setting at which you do not experience airway obstructions. We take a closer look at how this setting is determined and why it might be adjusted over time.
Determining CPAP Pressure Settings
Doctors and sleep specialists use the term “titration” to describe the process of determining CPAP pressure levels. The main goal of CPAP titration is to identify the lowest amount of air pressure needed to reduce snoring, shallow breathing, interruptions in breathing, and the sleep disturbances they cause.
Many people have their initial CPAP pressure settings established during a sleep study, also called polysomnography. The sleep study can be either an all-night session for titration or a split-night sleep study, which includes both sleep apnea diagnosis and CPAP titration. Titration during a sleep study is generally considered the most accurate way to decide CPAP pressure levels.
CPAP pressure is measured in centimeters of water pressure, or cm H2O. During a sleep study, a sleep technician begins with a low pressure level, often 4 cm H20. Then they increase the pressure by 1 or 2 cm H20 every 5-10 minutes until there is no more obstruction in the upper airway.
Many health professionals consider 20 cm H20 to be the maximum CPAP pressure level. The majority of people who use CPAP for sleep apnea have pressure levels set at between 8 and 10 cm H20. But your specific setting will depend on a number of factors.
Following the sleep study, your health care provider may also fit you with a mask and offer instruction for using the CPAP machine at home. Your doctor will revisit your CPAP pressure, mask fit, and sleep apnea symptoms during follow-up visits and calls over the next several weeks.
At-Home Titration
In certain cases, CPAP pressure levels can be determined at home using an auto-adjusting positive airway pressure (APAP) device. An APAP detects breathing obstructions during sleep and automatically increases or decreases air pressure as needed. This approach may be an option for people with moderate or severe OSA who do not have other respiratory disorders.
Home titration with an APAP generally takes place over days or weeks. Its aim is to find the pressure levels that eliminate breathing obstructions for at least 90% to 95% of the sleep period. These levels, known as P90 and P95, are recorded by most APAP machines.
Doctors use your P90 and P95 levels as starting points for determining the fixed setting for CPAP pressure. After examining the data from the collection period and reassessing your symptoms, they make adjustments to the pressure levels and may adjust them further at follow-up visits.
APAP titration can help health care professionals determine the optimal CPAP pressure level, but it cannot be used to diagnose sleep apnea.
Factors That Can Affect Pressure Settings
When determining CPAP pressure settings during a sleep study, doctors and sleep specialists consider the severity of your sleep apnea, as well as a variety of sleep quality measurements.
Doctors determine the severity of your OSA using the apnea-hypopnea index (AHI). Your AHI can be mild, moderate or severe depending on the number of times per hour of sleep that you partially or completely stop breathing.
Several factors may be included in a specialist’s determination of CPAP pressure settings.
- Body weight: People who weigh more may need higher pressure settings, while having a lower weight might allow for lower settings.
- Anatomy: A person’s head and jaw shape, neck circumference, and the size of their tongue and tonsils can all affect the degree of airway obstruction.
- Sleep position: People with sleep apnea who sleep on their backs may require higher CPAP pressures than those who sleep on their sides.
- Sleep stages: A person’s AHI may fluctuate based on each sleep stage. The sleep specialist will observe the person during each stage of sleep to determine which pressure level will keep their AHI the lowest and prevent awakenings during REM sleep.
In addition to these, a doctor will take into account features of your lifestyle, overall health, and other health conditions you may have.
How to Know if Your CPAP Pressure Needs Adjusting
When you first start using a new CPAP device, you can expect frequent adjustments to your pressure settings. Your doctor will make these changes based on sleep data from the first weeks that you use the machine, as well as on the degree to which the treatment relieves your symptoms.
You will also have regular check-ins over the phone or in person to make sure there are no obstacles preventing you from using the device consistently and comfortably.
A well-fitting mask makes a great difference in the effectiveness of CPAP therapy. New CPAP users often try a number of different masks before finding the right fit. If you change the type of mask you wear after your initial titration, you may need to have your CPAP pressure settings adjusted.
You may also need readjustment of pressure settings if you continue to experience sleep apnea symptoms despite using your CPAP regularly. Persistent symptoms such as daytime fatigue, snoring, or a high number of respiratory events during the night can be signs that you should speak with your doctor.
To address your concerns, your doctor might reassess the fit of your mask, check for leaks, and adjust the pressure or other device settings. Your doctor will evaluate your symptoms again after two to four weeks.
In some cases, you might need to return to the laboratory for a new titration. But if your CPAP is equipped with a modem, your doctor may be able to adjust the pressure remotely. If adjusting your CPAP pressure level doesn’t help, your doctor or sleep specialist may also recommend a different type of device, such as an APAP or a bilevel positive airway pressure (BiPAP) machine.
Additional Settings
If you’re feeling discomfort from exhaling against the CPAP’s air pressure, your doctor might recommend a device with pressure relief. Pressure relief may ease this discomfort by lowering the air pressure when you exhale.
Another optional setting that may aid in CPAP use is called a pressure ramp. This setting addresses discomfort with pressure while you are falling asleep by allowing you to program a gradual increase in pressure over time. As you fall asleep over the course of 5 to 45 minutes, the device will reach the desired pressure level.
Side Effects if Your CPAP Pressure Isn't Right For You
CPAP titration is meant to identify the lowest pressure setting necessary to get results. This means that a higher CPAP pressure setting is not necessarily better.
Higher-than-necessary pressure levels can make breathing uncomfortable and could lead people to stop using their CPAP devices. Pressure that is too high can also cause mask leaks, making the therapy less effective. Too-high pressure can even contribute to another breathing problem called treatment-emergent central sleep apnea.
Meanwhile, if the pressure setting is too low, the CPAP may not be able to keep the upper airway sufficiently open during sleep. Your sleep may not improve, and you could end up experiencing the same respiratory disturbances and symptoms as before.
Benefits of Optimizing Your CPAP Pressure
Finding the best CPAP pressure level increases the likelihood that you will continue the treatment. Successful CPAP treatment can improve your sleep by decreasing the number of disturbances you experience. But long-term CPAP use can benefit your health in many other ways, including:
- Eliminating snoring
- Reducing daytime sleepiness
- Lowering the chance of a stroke
- Controlling blood pressure
- Improving memory and concentration
- Decreasing acid reflux
- Improving erectile dysfunction
Perhaps most importantly, controlling your OSA with CPAP could give you a longer lifespan. One study showed that people who continued their CPAP therapy for the full year after it’s prescribed had lower mortality rates in that time.
How to Change Your CPAP Pressure Settings
If you have concerns about your CPAP pressure settings, it’s important for you to speak to your doctor, rather than attempt to change the settings on your own. These settings should be changed only under the supervision of a trained medical professional.
Once the initial titration is complete, you can expect many check-ins and consultations with your doctor or sleep specialist in the weeks to follow. These are opportunities for your health care team to reevaluate your pressure settings and recommend adjustments as needed.
Keep communicating with your doctor about any discomfort you experience or sleep apnea symptoms you might still notice. Having your concerns addressed makes it more likely that your CPAP therapy will be worthwhile.
References
Ask the Sleep Doctor
Have questions about sleep? Submit them here! We use your questions to help us decide topics for future articles, videos, and newsletters. We try to answer as many questions as possible. You can also send us an email. Please note, we cannot provide specific medical advice, and always recommend you contact your doctor for any medical matters.