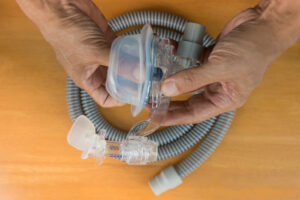
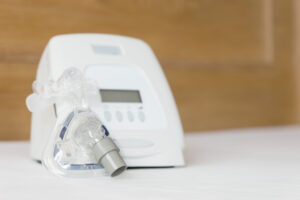
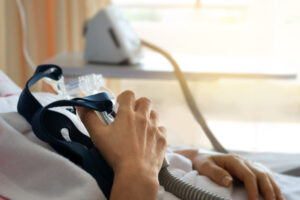
Both BiPAP and CPAP are types of positive airway pressure (PAP) devices that can be used to treat sleep apnea, a condition marked by paused or shallow breathing during sleep. PAP machines work by sending pressurized air through a hose into a mask worn on the face. This air helps keep the airway open and normalize breathing during sleep.
Different PAP machines function somewhat differently. Continuous positive airway pressure (CPAP) machines release a constant level of air pressure. Bilevel positive airway pressure (BiPAP or BPAP) machines release air at two different pressure levels, one for breathing in and one for breathing out.
For people with sleep apnea, nightly use of a PAP device can improve breathing and sleep. Knowing what distinguishes BiPAP from CPAP machines can help you understand these treatment options and how to make the most of PAP therapy.
Key Takeaways
- CPAP provides a constant air pressure to keep airways open and is effective for obstructive sleep apnea.
- BiPAP offers two pressure levels and is used for complex cases of sleep apnea.
- Different air pressure levels for inhalation and exhalation may be beneficial for people with shallow breathing or are experiencing difficulty exhaling with a CPAP.
- Your doctor will help you find the appropriate PAP therapy based on your condition and needs.
What Is BiPAP?
BiPAP stands for bilevel positive airway pressure. BiPAP works by sending pressurized air into the upper airway. This airflow keeps the airway clear of obstruction to prevent lapses in breathing, snoring, and sleep disruptions.
BiPAP treatment is provided using a bedside machine, which is usually small enough to fit inside a shoebox. The machine pressurizes air and pumps it through an attached hose. At the other end of the hose is a mask that is worn over the nose or the nose and mouth. Air flows through the hose and mask and into the upper airway that leads to the lungs.
When the BiPAP machine is turned on, it releases air at two different pressure levels. Inspiratory positive airway pressure (IPAP) refers to the level of air pressure delivered when a sleeper is breathing in. Expiratory positive airway pressure (EPAP) refers to the level of air pressure delivered when a sleeper is breathing out.
A BiPAP machine generally delivers higher air pressure while the sleeper is breathing in and lower air pressure while they are breathing out. The air pressure settings are calibrated carefully to try to make the BiPAP treatment as effective as possible at resolving breathing disruptions.
How Are BiPAP Pressure Levels Determined?
Experts recommend establishing BiPAP settings during a sleep study conducted in a specialized sleep lab. During the study, a technician can closely monitor breathing, oxygen levels, and brain activity. With this data, they can identify which BiPAP pressure levels have the best impact on a specific person’s breathing and sleep quality.
In addition, some BiPAP machines have built-in sensors that are designed to automatically adjust pressure levels to avoid breathing disruptions. These machines can also be used to determine the initial pressure levels. However, experts recommend initially determining optimal pressure levels in a sleep study, instead.
When the auto-adjusting BiPAP technology is used to determine air pressure levels, doctors often closely monitor data from the device and may recommend a follow-up sleep study to confirm that it is working.
How Is BiPAP Different From CPAP?
CPAP is typically the initial treatment for obstructive sleep apnea (OSA), which is the most common type of sleep apnea. However, BiPAP may be prescribed to certain people who have OSA, central sleep apnea, or another sleep-related breathing problem.
The key difference between BiPAP and CPAP is that a BiPAP machine provides different air pressure levels for inhalation and exhalation. In contrast, a CPAP machine uses the same amount of air pressure whether the sleeper using the machine is breathing in or out.
In many ways, though, the differences between BiPAP and CPAP machines are growing smaller. Often, contemporary CPAP devices are able to provide more than one level of air pressure. For example, a pressure relief setting on many CPAP devices allows for a minor reduction in air pressure during exhalation.
Two types of BiPAP machines are available, and the type of BiPAP machine a sleeper has impacts the air pressure they receive while asleep.
- Fixed BiPAP: In these machines, two fixed air pressure levels — one for breathing in and one for breathing out — are determined by a doctor and programmed into the device. These two levels do not change during the night.
- Auto-adjusting BiPAP: Auto-adjusting BiPAP devices can modify pressure levels in response to a sleeper’s breathing. While these BiPAP machines start with programmed base levels of pressure for breathing in and out, they use sensors to monitor breathing and an algorithm to alter pressure levels as needed.
Because auto-adjusting BiPAP devices are newer, there is limited data showing that they treat sleep apnea and other breathing problems as well as fixed BiPAP devices.
What Are the Benefits of BiPAP?
For people with obstructive sleep apnea, a major benefit of a BiPAP machine is that it may be more comfortable to use than a CPAP machine, because of the lower air pressure level it delivers during exhales.
People who require high levels of air pressure while inhaling may especially benefit from using a BiPAP machine. High air pressure might be difficult to tolerate while breathing out. By providing lower pressure during exhalation, a BiPAP machine may encourage nightly use, which is important for treating sleep apnea.
BiPAP machines can be programmed to operate in one of three different modes depending on what is needed to resolve breathing problems. Because a BiPAP machine can be programmed with a timer, BiPAP therapy can also offer benefits to people with health conditions that cause slowed or irregular breathing, including central sleep apnea. In these cases, BiPAP can help regulate breathing and enable better sleep.
What Are the Drawbacks of BiPAP?
When used for obstructive sleep apnea, the main concerns of using a BiPAP machine are the potential for insufficient pressure and higher costs.
By design, a BiPAP device lowers the level of air pressure during exhalation. For some people, it is possible that the pressure will be too low to keep the airway open and successfully treat obstructive sleep apnea.
Another potential drawback is that BiPAP machines can be more expensive than CPAP machines. People whose devices are covered by insurance may not notice a big price difference, but BiPAP therapy may have a larger financial impact on those who have to pay for their machine out of pocket.
Who Is BiPAP Best for?
Research studies have found similar results for both CPAP and BiPAP as treatments for obstructive sleep apnea (OSA). For most people with OSA, CPAP is initially recommended because of its simplicity and extensive track record. However, there are circumstances in which BiPAP therapy may be more effective than CPAP.
BiPAP machines are typically best for people who have complex sleep-related breathing problems or who have struggled with CPAP therapy. BiPAP therapy is most often used in two specific circumstances:
- If high pressure is required: Some sleepers need very high levels of air pressure when they inhale in order to prevent breathing disruptions. A BiPAP machine delivers this higher air pressure, then reduces the pressure level during exhalation.
- If initial CPAP therapy is ineffective: While CPAP helps many people with obstructive sleep apnea, it is not effective for everyone. In addition, some people are bothered by the air pressure provided by the CPAP device when they exhale. In these cases, a switch to BiPAP therapy may help improve breathing during sleep.
BiPAP is also often the best treatment option for people who have complicated breathing disorders. For example, BiPAP therapy may be prescribed to people with central sleep apnea (CSA), which is caused by improper signaling between the brain and the muscles that control breathing. In particular, BiPAP is often recommended for people with CSA tied to health issues that can cause slow or shallow breathing.
Since PAP machines are only available by prescription, the decision about whether to use BiPAP, CPAP, or another type of PAP therapy must be made by a doctor or sleep specialist.
How to Make the Most of BiPAP Therapy
To optimize BiPAP therapy, follow any directions provided by your doctor or sleep specialist. For example, a doctor might give guidance about the BiPAP machine’s settings, how often to use the machine, and how to keep it clean and operational. It may also be helpful to review any instructions from the device manufacturer about machine maintenance.
Using a mask that fits well and prevents air leaks is also important for successful PAP therapy. It is normal to try multiple masks before finding the best option, so talk with your doctor if the first mask you are given feels uncomfortable or leaks air.
If you experience any problems with the BiPAP machine, challenges with the mask or other accessories, or persistence of breathing problems or other symptoms, talk with your doctor or sleep specialist about potential solutions.

When to Consider Other Breathing Machines
Although a BiPAP machine can be beneficial in many circumstances, it is sometimes necessary to consider other breathing machines.
For example, if you have obstructive sleep apnea without any other breathing problems, a CPAP machine is likely to be recommended for starting treatment. BiPAP therapy may also not be appropriate for people with central sleep apnea and certain underlying health issues, including some types of heart failure.
If you have already started using a BiPAP machine, you and your doctor may consider another type of breathing machine if you do not see an improvement in your symptoms. Your treatment plan may also be modified if you have had any recent changes to your symptoms or overall health.
Frequently Asked Questions About BiPAP vs. CPAP
An auto-adjusting positive airway pressure (APAP) device operates similarly to a CPAP device, but modifies the levels of air pressure delivered in response to changes in breathing. Auto-adjusting technology can also be integrated into a BiPAP device, but BiPAPs are frequently prescribed with fixed air pressure settings.
APAP devices are also known as auto-CPAPs, and they may be used as an initial treatment for people with obstructive sleep apnea that do not have other breathing disorders or difficulties. BiPAP machines are generally not first prescribed for obstructive sleep apnea. Instead, BiPAP therapy is often tried when a person with OSA cannot tolerate CPAP or APAP treatment.
In most cases, a BiPAP machine is more expensive than a CPAP machine. However, the actual out-of-pocket cost depends on your health insurance coverage, including whether you have required copays or deductibles
Although there can be some variation based on the brand and model, most BiPAP and CPAP machines are around the same size. These devices can usually fit on a nightstand to provide easy access during the night
A prescription is required to obtain a BiPAP machine or other type of PAP therapy. For this reason, it is important to talk to a doctor or sleep specialist about any concerns related to breathing during sleep. A sleep test is often the next step.
Many BiPAP devices include a pressure ramp feature. The ramp function allows for a lower level of air pressure to be delivered during the first 5 to 45 minutes of use after which the device begins to pump at its full prescribed pressure.
The effectiveness of BiPAP therapy is determined by tracking changes in your symptoms and by checking information that is recorded by the device. BiPAP machines collect data about your breathing during sleep, and your doctor can review this data to see how well the BiPAP is improving your breathing problems.
References
Ask the Sleep Doctor
Have questions about sleep? Submit them here! We use your questions to help us decide topics for future articles, videos, and newsletters. We try to answer as many questions as possible. You can also send us an email. Please note, we cannot provide specific medical advice, and always recommend you contact your doctor for any medical matters.