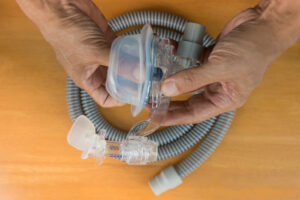
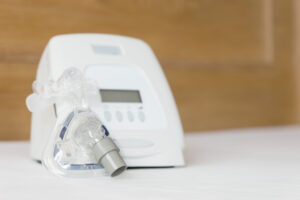
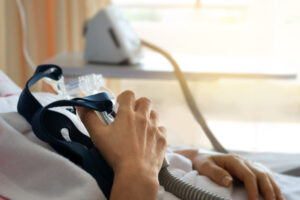
Different kinds of positive pressure airway (PAP) machines can be used to treat sleep apnea, a common condition that involves short interruptions of breathing during sleep. PAP machines promote uninterrupted breathing by sending a stream of pressurized air through a mask and into the upper airway that leads to the lungs.
Auto-adjusting positive airway pressure (APAP) and continuous positive airway pressure (CPAP) devices are both methods of providing PAP therapy, but there are important differences between them. A CPAP machine produces a flow of air with a steady amount of air pressure, while an APAP machine automatically modifies the air pressure level to match breathing patterns during sleep.
Knowing the similarities and differences between APAP and CPAP can help you understand the possible benefits and drawbacks of both devices and allow you to talk with your doctor about what type of sleep apnea treatment is right for you.
What Are CPAP and APAP?
A CPAP machine works by continuously pumping pressurized air into your airway during sleep. An APAP machine is different because it uses sensors and built-in software to make automatic changes in air pressure in response to your breathing.
Despite this difference, APAP may be called auto-CPAP. Even though an APAP can modify the amount of air pressure delivered, it is similar to a CPAP in that it usually maintains the same level of air pressure during inhalation and exhalation.
Both APAP and CPAP devices are frequently used as treatments for obstructive sleep apnea, a condition in which tissues in the mouth and throat block the upper airway and disrupt breathing during sleep. These devices generate a flow of pressurized air that keeps the airway open and allows for normal airflow.
Many of the same extra features are found on APAP and CPAP machines.
- Heated Humidification: This method of reducing mouth or nose dryness involves adding moisture to the stream of air by heating up water from an attached reservoir.
- Pressure Ramp: This feature allows the device to gradually build up to full air pressure, which may make it easier to fall asleep while using their PAP machine.
- Pressure Relief: With a pressure relief feature activated, the machine slightly decreases the amount of air pressure when you breathe out, making it easier to exhale.
Both APAP and CPAP machines are kept by the bedside and involve similar components, including a hose and mask, to deliver air into the upper airway. In addition, both types of machines require a prescription.
How Is APAP Different From CPAP?
An APAP machine automatically adjusts the level of air pressure provided and may change these levels many times during the night. In contrast, a CPAP provides a constant stream of air that maintains a consistent amount of pressure during sleep.
The benefit of an APAP is most clear in someone whose sleep apnea symptoms tend to vary from night to night or during any given night.
For example, some people may have breathing disruptions primarily when they sleep on their back. With a CPAP, the device pumps air at the same pressure regardless of their sleeping position. An APAP, though, uses sensors to assess breathing, allowing it to increase the pressure when someone rolls onto their back and starts having breathing lapses.
Another difference between CPAP and APAP relates to how the devices are configured. The air pressure levels on a CPAP are set by a sleep specialist during an overnight sleep study, but an APAP allows for these levels to be determined by the machine’s algorithms while being used at home.
By design, CPAP machines are generally simpler than APAPs. CPAP therapy also has a longer history of effectively treating obstructive sleep apnea. While the use of APAP machines is growing, CPAPs remain the most common initial treatment because of their track record, familiarity, and ease of use.
Who Should Consider APAP?
APAP machines may be recommended as an initial treatment if you have mild to severe obstructive sleep apnea without complications. Complications that might be a barrier to using APAP include heart failure, central sleep apnea, and other conditions that affect the lungs or breathing.
CPAPs therapy remains the most frequently prescribed first treatment for obstructive sleep apnea, but APAP may be an option for some people who are just starting treatment. APAP may be especially convenient if you live far away from a sleep clinic or otherwise have difficulty going in for a sleep study to determine CPAP settings.
APAP therapy may be suggested if you have notable variability in the severity of your symptoms of obstructive sleep apnea. Because it can adjust pressure in real-time, an APAP machine may be more suitable if your breathing during sleep changes based on specific circumstances.
- Weight Fluctuations: Obstructive sleep apnea may worsen if you gain weight and improve if you lose weight. An APAP can adapt to new air pressure requirements caused by weight changes.
- Body Position: The tissue in the throat is more likely to block the upper airway when lying on your back. The upper airway is more likely to stay unobstructed when sleeping on your side. If you adjust your sleep position at night, an APAP may detect changes in breathing and start pumping air as necessary to prevent breathing lapses.
- Alcohol Consumption: Drinking alcohol prior to bedtime can make sleep apnea worse, while avoiding alcohol may improve symptoms. If you drink occasionally, you may find an APAP device most effective for your lifestyle as it can adapt to meet changing pressure needs tied to alcohol intake.
- Recurrent Allergies: Nasal congestion from allergies may worsen sleep apnea symptoms, so APAP therapy may be helpful if you have episodes of allergies that affect your breathing.
APAP can also be prescribed if initial treatment with a CPAP machine is not successful. For example, an APAP may be recommended if you find it difficult to tolerate the constant pressure of a CPAP machine despite trying other things to make it more comfortable.
Are There Drawbacks to APAP?
Research has generally found CPAP and APAP to be equally effective for most people with obstructive sleep apnea. However, there is less evidence proving the effectiveness of APAP, which is a newer and more variable technology, than there is for CPAP, which has been in use for over 40 years.
Additionally, APAP is not suitable for people who have obstructive sleep apnea that coexists with certain other health conditions. APAP is usually not a good choice of therapy for people with obstructive sleep apnea who also have:
- Severe chronic obstructive pulmonary disease (COPD)
- Congestive heart failure
- Central sleep apnea
- Obesity hypoventilation syndrome
- Regular use of certain drugs, including opioids and anti-seizure drugs
APAP is also not usually a viable treatment option for people who have difficulty maintaining a good seal between the mask and their face when using a PAP machine. If air leaks out of the mask, the APAP may not properly calibrate the amount of pressure to provide. At-home setup of an APAP may also not be possible for people who want to easily experiment with multiple types of masks.
In addition, there are other potential drawbacks of APAP that may affect certain people.
- Insufficient Pressure: While APAP has generally been shown to be effective, there is a risk that the device could auto-adjust in a way that fails to provide enough air pressure to resolve breathing disruptions. This could occur from a mask leak or a problem with the device’s sensors or software.
- Too Much Pressure: If an APAP’s algorithm causes the machine to pump air that is overpressurized, it could contribute to breathing problems during sleep.
- Disruption From Pressure Changes: Some people may notice when the APAP changes air pressure levels, which may be bothersome during sleep.
- Higher Cost: APAP machines are typically more expensive than CPAPs, increasing costs for people whose insurance is not covering the full cost of their treatment for obstructive sleep apnea.
- Reduced Control of High Blood Pressure: Although not definitive, some research has found that fixed-level CPAP is better at decreasing high blood pressure than APAP.
A doctor or sleep specialist can explain whether APAP is an option and can discuss how it compares to other types of treatment, including CPAP.
Frequently Asked Questions About APAP vs. CPAP
Treatment with APAP may result in many of the same side effects as CPAP treatment. These include nasal stuffiness, dry mouth, or a sore throat upon awakening. However, some people find that APAP is less likely to cause discomfort from the flow of pressurized air into the mask.
APAP devices are also known as auto-CPAPs, and they may be used as an initial treatment for people with obstructive sleep apnea that do not have other breathing disorders or difficulties. BiPAP machines are generally not first prescribed for obstructive sleep apnea. Instead, BiPAP therapy is often tried when a person with OSA cannot tolerate CPAP or APAP treatment.
In general, APAP is significantly more expensive than CPAP. The cost of a CPAP machine, not including accessories like masks and hoses, ranges from $500 to $1,000. An APAP device usually costs more, with its price ranging from $1,700 to $3,000.
The exact amount that you have to pay for an APAP or CPAP machine can depend on the brand and model as well as whether you have insurance that is covering some or all of the costs of the machine.
APAP is often covered by insurance if you have been diagnosed with obstructive sleep apnea. However, you should always check with your insurance provider directly for specific information about coverage and out-of-pocket costs.
In addition, your insurance carrier may make you demonstrate that you need APAP treatment and may require information from your doctor showing that you are benefitting from an APAP device. Your insurance provider may also ask to review data from the APAP device that proves you are using it as directed.
References
Ask the Sleep Doctor
Have questions about sleep? Submit them here! We use your questions to help us decide topics for future articles, videos, and newsletters. We try to answer as many questions as possible. You can also send us an email. Please note, we cannot provide specific medical advice, and always recommend you contact your doctor for any medical matters.