A continuous positive airway pressure (CPAP) machine pumps pressurized air through a hose and mask, allowing this stream of air to reach the windpipe and keep it open during sleep. CPAP machines are used to treat a sleep disorder called sleep apnea.
While CPAP machines can often eliminate the symptoms of sleep apnea, many people feel overwhelmed or intimidated when starting CPAP treatment. There are many CPAP machines on the market, and some can be expensive. In addition, the process of setting up and getting used to a CPAP machine may seem complicated or challenging.
There is often a learning curve in beginning CPAP treatment, but for people with sleep apnea, regularly using a CPAP can promote better sleep and deliver many important physical and mental health benefits.
Top 5 CPAP Tips

- 1 Try different masks to find the right mask for your face.
- 2 Try the ramp function to gradually increase air pressure as you sleep.
- 3 Talk to your provider about adjusting air pressure as needed.
- 4 Address nasal congestion for improved CPAP treatment.
- 5 Use a humidifier to prevent dryness and irritation.
Getting used to a CPAP machine can take a while, but asking about adjustments and cleaning your equipment may help to reduce discomfort.
How Do CPAP Machines Work?
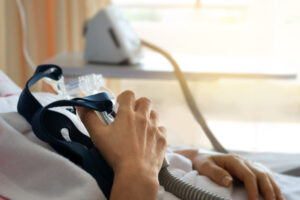
The goal of a CPAP machine is to provide a steady stream of pressurized air that keeps the windpipe open during sleep.
To accomplish this, a CPAP machine continuously pumps air set to a specific pressure level through a hose that is attached to a mask. The mask is worn around the nose and/or mouth during sleep.
The constant stream of air from the CPAP holds the airway at the back of the throat open. This is important for people with obstructive sleep apnea, a sleep disorder that causes temporary pauses in breathing when the airway becomes blocked.
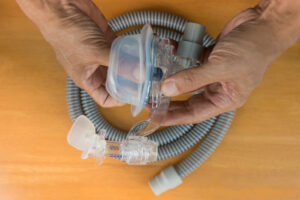
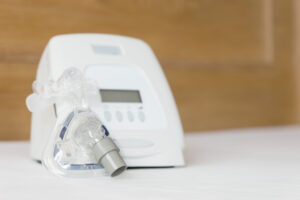
Components of CPAP Machines
Although CPAP devices come in many models and styles, most include the following parts:
- Machine: A CPAP machine’s base unit contains a motor that blows pressurized air through a filter and into a hose. Some models include a built-in humidifier and may have a “ramp” setting to allow the air pressure to gradually increase. Most people keep the machine beside or under their bed.
- Filter: CPAP machines contain either one or two filters, which typically must be cleaned or replaced periodically. Filters purify the air before it enters the mask.
- Tubing: A hose or tube allows air to travel from the CPAP machine’s base unit into the mask. CPAP tubing should be inspected regularly and replaced when necessary.
- Mask: A mask carries pressurized air from the hose into the nose and/or mouth so that it can reach the airway. Masks can be made from different materials like plastic, silicone, vinyl, or a gel-like material. Masks usually come with straps or other headgear to hold the mask in place.
- Humidifier: Many CPAP machines have a built-in humidifier chamber that can be refilled with water. Some studies suggest that tap water can be used, but the device manufacturer may recommend using sterile water, such as distilled water.
Types of CPAP Masks
CPAP masks come in a variety of shapes, designs, and materials depending on whether they provide pressurized air through the nose, mouth, or both. A mask must fit properly, creating a seal against the face and preventing air from leaking out around it.
The right type of CPAP mask varies from person to person based on multiple factors, including comfort preferences, sleeping position, air pressure requirements, and breathing patterns. Some models include extra options like cushions or adjustable components. Usually, a health care provider will help you select a mask to try initially.
Most CPAP masks fall into one of the following categories.
| Type of Mask | Design | Considerations |
|---|---|---|
| Nasal | Covers the nose and may include prongs that fit directly into the nostrils. | Can be used with higher pressure levels and comes in a wide range of sizes and shapes to suit most people. |
| Full-face | Covers the entire nose and mouth and, less commonly, the eyes as well. | Works well for people who require a high level of air pressure and for people who often breathe through their mouth. |
| Oral | Covers the mouth only. | Designed primarily for people who breathe through their mouth at night. |
| Nasal pillow | Sits under the nose and seals over each nostril without covering the whole nose. | Compact and sometimes more comfortable, but may not work for people who need a high level of air pressure. |
Benefits of CPAP Machines
CPAP is often the best treatment for obstructive sleep apnea. People who use their CPAP machines consistently and correctly report significant improvement in their quality of life. Many people feel better after just one day of using a CPAP machine, and some begin to develop normal sleep patterns in about one week.

CPAP treatment can make sleep more restful, reducing daytime sleepiness. Using a CPAP can reduce snoring which may improve a bed partner’s sleep as well.
In addition, consistently using a CPAP is associated with other health benefits in people with obstructive sleep apnea:
- Improved memory and concentration
- Better mood and fewer symptoms of depression
- Reduced anxiety
- Lower blood pressure
- Greater insulin sensitivity
Side Effects of CPAP Machines
Although there are many benefits to using a CPAP machine, there are also some drawbacks. For some people, these issues can make it challenging to use a CPAP machine on a regular basis.
Is it estimated that up to 40% of people who are prescribed CPAP therapy do not use the machine. This may be because the machine or mask makes them feel anxious, claustrophobic, or uncomfortable. The stream of pressurized air can also cause the mouth or throat to feel dry.
Other potential side effects of using a CPAP include:
- Stuffy or runny nose
- Nosebleeds
- Skin irritation around the nose or mouth
- Irritated eyes
- Muscle pain in the chest
- Difficulty tolerating higher air pressure levels
The types of effects can vary based on the type of mask being used, the model of CPAP device, and the air pressure level.
Many problems occur only the first few times a person uses their CPAP machine and go away with repeated use. Persistent issues can be prevented or remedied. Make sure to talk with your doctor about any issues or concerns you’re experiencing so that they can help you address them.
Adjusting to Using a CPAP Machine
Getting used to a CPAP machine can take a while, and it may be tempting to give up on treatment when struggling with side effects. However, the benefits of CPAP therapy typically outweigh the drawbacks.
A doctor can often suggest approaches to help get used to the CPAP. Some specific tips for adjusting to a CPAP machine include:
- Consider a different mask: The optimal mask depends on the individual, so finding the right mask can make using a CPAP easier. For example, people who are claustrophobic and dislike wearing a large mask can ask their health care provider about a smaller mask or a nasal pillow mask.
- Try the ramp function: Some CPAP machines have a “ramp” setting that gradually increases air pressure after starting the device. This allows many people to fall asleep more easily before the CPAP’s air pressure increases.
- Ask about air pressure: The CPAP’s air pressure level is set based on specific individual measurements, but if the air pressure feels too strong or too weak, it can be worthwhile to ask about an adjustment.
- Get treatment for nasal congestion: If CPAP is causing a stuffy nose, a saltwater spray may offer relief. A doctor or pharmacist may also be able to recommend cold or allergy medicines that may be helpful.
- Harness humidity: Many users complain of dry eyes, skin, and nasal passages when using a CPAP. Some CPAP machines come with a water chamber to humidify the air before it is delivered to the mask. In addition, using a humidifier for the entire bedroom may reduce problems with dryness.
It is important to remember that it is normal to struggle with a CPAP at the start. Getting advice from a doctor or sleep specialist can reduce bothersome effects, make sure the equipment is working properly, and help you reap the benefits of nightly CPAP use.
Tips for Selecting the Right CPAP Machine for You
CPAP therapy is intended for consistent use night after night, which means that it’s important for your CPAP device and mask to match your needs. Several approaches can help you select a CPAP machine and make sure it is the best fit for your situation.
Communicate With Your Health Care Provider
A prescription is required to receive a CPAP machine. Your doctor can write this prescription and may help you choose a CPAP model. It is important to be open with your doctor and bring up any preferences or concerns that you have about CPAP therapy.
For example, you should let your doctor know if you are allergic to certain materials, breathe through your mouth when you sleep, or feel anxious in small spaces. Your doctor can steer you towards a quality CPAP machine that suits your sleeping style and comfort needs.
Once you choose a CPAP machine, you should maintain communication with your doctor, especially if you are experiencing side effects, still having symptoms of sleep apnea, or struggling to continue CPAP therapy. Your doctor may be able to find another option that works for you.
Choose the Right Mask
A comfortable mask with a good seal is vital to successful CPAP treatment. A mask that is too loose may leak air, while overly tight masks may be uncomfortable or cause irritation.
As you explore your options, keep your preferences and typical sleep habits in mind. Things that can impact a mask’s fit and overall feel include your sleeping position, whether you move in your sleep, and even whether you have facial hair or wear eyeglasses.
You may be able to test out different types or brands of masks to find one that works well for you. You can also try a mask with comfort options like special cushioning or padding.
Find Out What Kind of Pressure You Need
Most people find out what air pressure they should use after they undergo a sleep study in a sleep center or take a sleep apnea test at home. There, a doctor or technician carefully monitors their breathing to find the ideal pressure level for keeping the airway open.
Using the wrong level of air pressure can be uncomfortable or make CPAP treatment ineffective. In addition, an ill-fitting CPAP mask may lead to excess snoring or breathing difficulties, which can cause insufficient sleep and daytime sleepiness. Contact your health care provider if you think that you may need to adjust your CPAP pressure level.
Consider Your Budget
Often, health insurance providers including Medicare will cover some or all of the costs associated with your CPAP machine. Some machines can be expensive, so it is important to find out what insurance will pay for before choosing a model.
CPAP Cleaning Guidelines
Regular maintenance is essential for keeping your equipment hygienic. Be sure to check the owner’s manual for specific cleaning instructions before using your CPAP machine for the first time. You’ll likely need to clean:
- Your nose pillows or cushions daily
- Your mask daily or every other day
- Your headgear, tubing, reusable filter, and humidifier chamber weekly
- Your CPAP machine as needed
Some companies sell devices designed to clean CPAP machines using ozone gas or ultraviolet light. However, the Food and Drug Administration has issued a warning about these devices. People who have used these types of CPAP cleaners report asthma attacks, headaches, and breathing problems. These devices are not approved by the FDA.
Frequently Asked Questions About CPAP Machines
After getting a prescription from your health care provider, you may purchase a CPAP machine online or at a brick and mortar store. If Medicare is fully or partially covering the cost of your CPAP treatment, you must buy your machine from a supplier who is enrolled in Medicare.
Your doctor or insurance plan may help you find a company that provides different types of CPAP machines and accessories. CPAP machines are not available for purchase without a prescription.
Prices vary considerably between CPAP machines. A CPAP machine may cost as little as $500 or more than $1,000, depending on the model and the type of pressure it administers.
Machines with advanced features typically cost more than basic models. How much you ultimately pay out of pocket for your CPAP machine also depends on whether it is covered by your health insurance or Medicare.
CPAP machines can be used to treat some conditions besides obstructive sleep apnea. CPAP therapy can be helpful in addressing some health problems that affect breathing and the ability of the lungs to get enough oxygen.
For instance, CPAP therapy may help some people with chronic obstructive pulmonary disease (COPD), respiratory failure, or heart failure. CPAP has also been studied in the treatment of people hospitalized with COVID-19.
CPAP is generally the initial treatment for obstructive sleep apnea, but it is not the only type of positive airway pressure (PAP) device. Other PAP devices use different methods to help keep the airway open.
CPAP: CPAP therapy uses a steady, constant amount of air pressure. That pressure level does not change when inhaling and exhaling.
Bilevel positive airway pressure (BiPAP): Unlike CPAP, BiPAP utilizes two pressure levels. With a BiPAP, air pressure levels are higher when inhaling and lower when exhaling.
Autotitrating or adjustable positive airway pressure (APAP): APAP, also called auto-CPAP, machines adapt to the user’s breathing patterns, adjusting pressure as needed throughout the night.
Doctors may prescribe BiPAP or APAP machines for people who find CPAP treatment uncomfortable or have other specific needs that are best met with another type of PAP